Kristen Haase, University of British Columbia and Don D. Sin, University of British Columbia
This holiday season, we are all itching for a little bit of normalcy. For many, this means spending time with family and friends, and dropping the masks to drink eggnog. But even if you are fully immunized against COVID-19 (whether that’s defined as two or three vaccines is currently under debate), the infectiousness of SARS-CoV-2, the virus responsible for COVID-19, means that you can still transmit the virus to others.
Vaccination is the best way to protect yourself against COVID-19. Even if infected, vaccinated people are less likely to have symptoms and more likely to have a mild course of infection. However, this means that you may not even know that you have SARS-CoV-2 (whether the Delta variant or Omicron) and could unwittingly pass it on to someone else.
To protect the most vulnerable — including those who are immunocompromised, the elderly and kids who have yet to be vaccinated — rapid antigen testing (rapid testing) is an extra measure that can help you have a more normal holiday, if used correctly. As health-care professionals, we have been involved in rapid testing research and clinical use during the pandemic. Here are some common questions and answers.
1. What is a rapid test?
Rapid antigen tests detect whether your body is shedding the SARS-CoV-2 virus. Rapid tests are very easy to use — so easy that an eight-year-old can become well-versed in the correct procedure and teach adults how to do it.
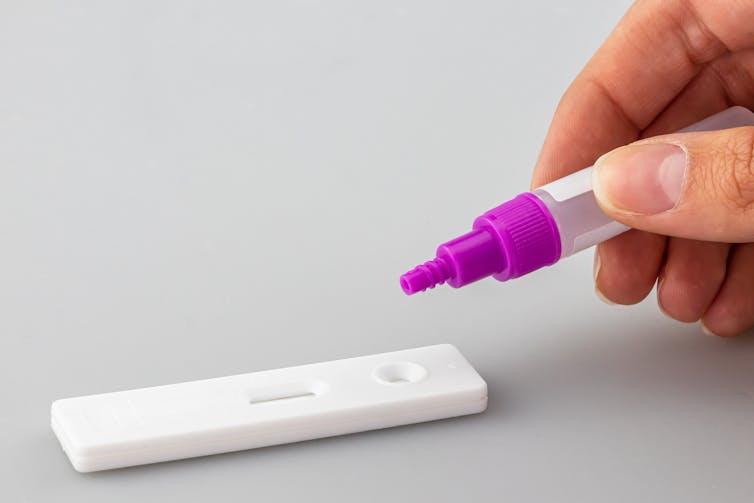
For most tests, you insert a stick resembling a cotton swab into each nostril for five seconds, roll it around and then mix it with a liquid solution. Then, using a dropper, you place the solution on a test kit (it looks like a pregnancy test). The result is ready in about 15 minutes.
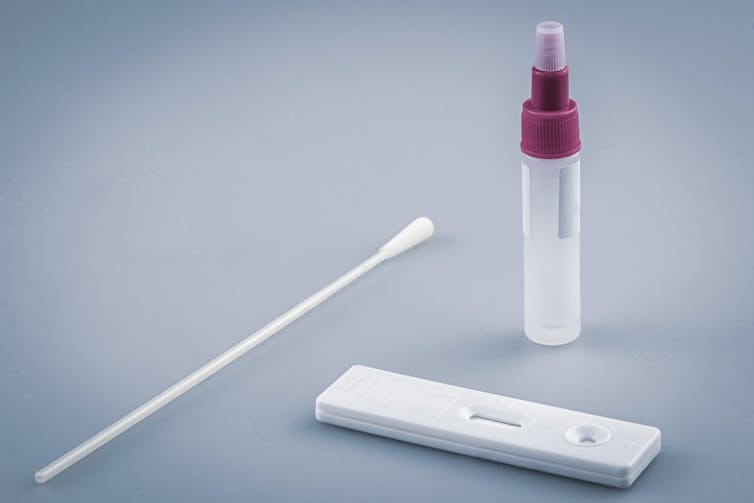
A rapid test differs from the PCR (polymerase chain reaction) test, which measures amplified viral RNA. PCR tests are generally more invasive. The sample is collected by a nasopharyngeal swab that requires sampling of nasal and pharyngeal pathways near the back of the throat. It takes longer to get results (hours to days versus minutes) and typically needs to be administered and processed by a health-care professional. However, the PCR test is the only choice if you are symptomatic and require a diagnosis at hospital or clinics.
2. What does a rapid test actually tell you?
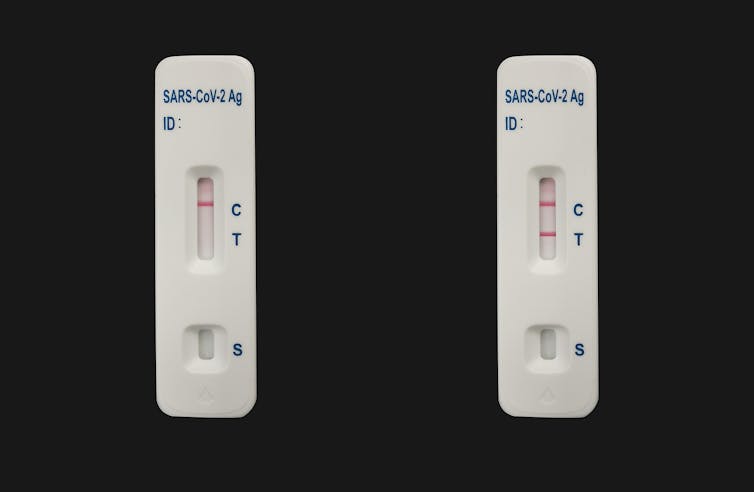
A rapid antigen tests tells you if you have the SARS-CoV-2 virus and are infectious in the moment — even when you are showing no symptoms (asymptomatic).
3. How long before an event should I take a rapid test?
A rapid test result is considered valid for the day you receive the results. So, it is most useful if you take the test shortly before you plan to attend an event or be in close quarters with others.
But you should be strategic about when you do it. For example, if you’re travelling four hours to see grandma for Christmas you likely want to take the test before you get in the car, because if you show up at grandma’s, take the test and find you’re positive, human nature might make you both want to bend the rules and have just a quick visit.
With the infectiousness of the Delta variant and, possibly, Omicron, this is not a safe choice.
If you have access to multiple tests and can test regularly — before you travel, before you interact with different groups of people on the same day — that is ideal.
4. When should I not use it?
Rapid tests should not be used when you are symptomatic and require a clinical diagnosis. Why? Because if you are symptomatic, you should self-isolate and/or get a PCR test, depending on your local guidelines and your personal vaccine status.
Your symptoms might not be related to COVID-19. They could also be due to the influenza virus, which could still be harmful to pass on to the immunocompromised. If you’re feeling unwell, stay home and get a PCR test in accordance with your local guidelines. Period.
5. How much does it cost? Where can I find one?
In Canada, many small businesses have cropped up to provide rapid tests for travel with costs ranging from $75-130. But tests can also be purchased individually or by the box starting at $10 per test.
Publicly funded tests are harder to come by, and availability varies by jurisdiction. The federal government gave rapid tests to each province, but how these are being shared varies widely.
Pop-up rapid test distribution centres have emerged in B.C. communities with high rates of COVID-19 through the Fraser Health Authority. Saskatchewan has been distributing rapid tests through business-lobby groups and schools, but has found that many people don’t know how to use the tests correctly. In Nova Scotia, infectious disease expert Dr. Lisa Barret has led a number of successful efforts to distribute rapid tests in the community, including giving out condoms and COVID tests to university students.
The bottom line
The best ways to protect yourself and your family from COVID-19 are to get vaccinated, wear a mask, keep your distance and gather outside when possible. If you choose to gather in person, rapid tests are one more tool in our toolbox to stay safe for the holidays. Remember, rapid tests aren’t for those with symptoms — they are only for people who are asymptomatic.
Kristen Haase, Assistant Professor, Nursing, University of British Columbia and Don D. Sin, Professor of Medicine, University of British Columbia
This article is republished from The Conversation under a Creative Commons license. Read the original article.

